Restech Continues to ‘Rethink Reflux’ with Acquisition of Somna Therapeutics
June 23, 2020
New French Distribution Agreement with Larylab® Technologie EIRL
September 11, 2020Pure Alkaline Pharyngeal Reflux after Nissen Fundoplication Surgery
By: Dr François Bobin ENT, Reflux Specialist
Sleep Center Polyclinique de Poitiers (France)
Click here to download a PDF of this case study
CASE HISTORY & EVALUATION
A 66-year-old male who worked as a retired school principal presented to the clinic. He is a non-smoker with a BMI = 24, who underwent laparoscopic Nissen fundoplication (anti-reflux surgery) in 1996. For several months following surgery he experienced digestive problems (including abdominal pain and diarrhea), pharyngeal irritation without dysphonia or oral burns, associated with frequent nocturnal awakening, and slight drowsiness (Epworth 8) without snoring.PPIs (esomeprazole, 40 mg once per day) were provided for two months as an initial treatment but proved ineffective.The patient’s RSS score upon presentation was 37 (8 + 29 + 0) with a significant LPR threshold > 131Upon visual inspection, larynx and pharynx appeared almost normal, though there was a small sliding 1 cm hiatal hernia demonstrated by digestive fibroscopy.
DIAGNOSIS AND TREATMENT
 Many questions arose: Is this a case of Obstructive Sleep Apnea (OSA)? Is there a potential relationship with LPR or residual post-surgery GERD? Had the patient’s diet and lifestyle compromised his, initially promising, anti-reflux procedure over the intervening years?
Many questions arose: Is this a case of Obstructive Sleep Apnea (OSA)? Is there a potential relationship with LPR or residual post-surgery GERD? Had the patient’s diet and lifestyle compromised his, initially promising, anti-reflux procedure over the intervening years?
MII-pH and polysomnography were performed simultaneously with Peptest.
• Peptest results were negative (one sample in the morning with an empty stomach <14 ng/ml, and one in the evening, after dinner, <14ng/ml).
• PSG showed a slight OSA (IAH 17/h).
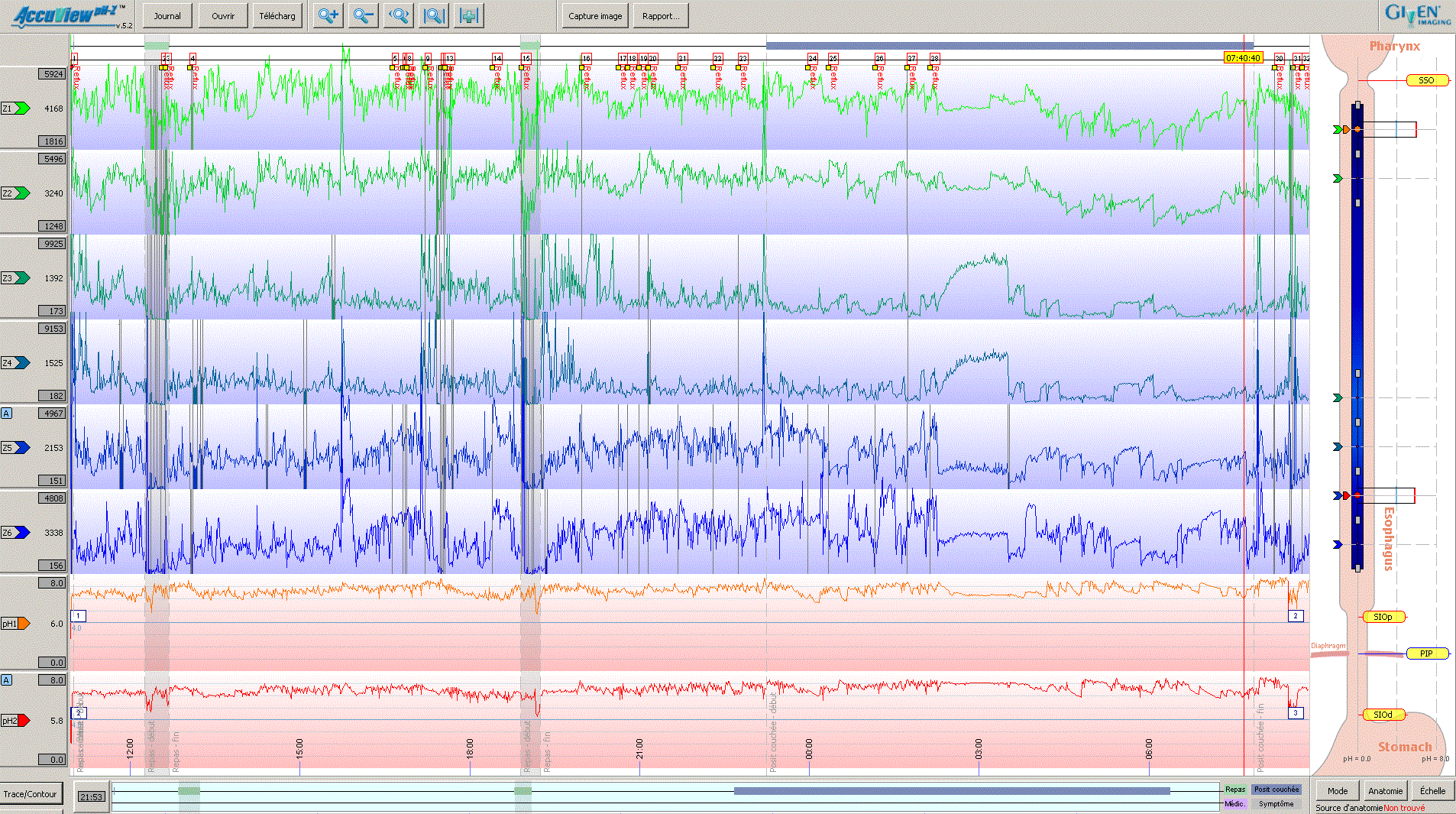
• MII-pH (performed off PPI) showed frequent episodes of non-acid reflux, distal (pH between 5.7 –7.2) and proximal (pH between 6 –7.5), throughout the day and at the beginning of the nocturnal period.
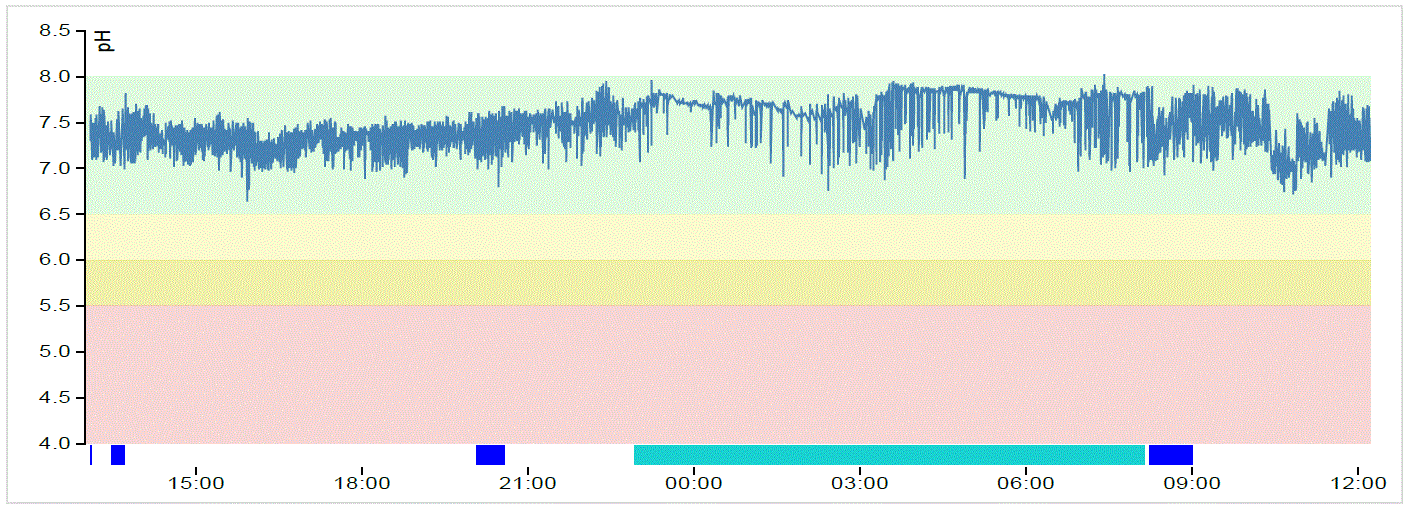
Pure non-acid reflux is a very rare occurrence but may be related to Nissen surgery. A Restech Dx-pH test was performed off PPI to measure the presence of any acid or non-acid reflux in the pharynx. The test showed a very wide amplitude indicating daytime alkaline reflux, with pH ranging between 7–7.8, but was less marked at night. The RYAN Score was normal (0 for both upright and supine), confirming that no acid reflux was present.
An adapted treatment was implemented for a non-acid reflux regimen, using Sucralfate (bile chelator) three times a day, one hour after eating.
The symptomatology improved after a few days. The RSS score one month later was 13 (4 + 9 + 0), a decrease of 24 points.
OUTCOME AND CONCLUSION
Bile reflux was probable, according to the negative Peptest excluding pepsin as a cause of symptoms. Alkaline reflux was revealed using the MII-pH and Restech Dx-pH tests and confirmed as symptomatology quickly improved following the introduction of Sucralfate.
The clinical utility for Restech’s Dx-pH System in diagnosing alkaline reflux is demonstrated in this case. Otolaryngologists often find these patients more complex than conventional GERD or LPR patients as true alkaline reflux cases are comparatively rare and there are limited diagnostic tools available. With further refinement, it is clear that this patient community can be better served through a more extensive diagnostic framework incorporating the Restech Dx-pH.
TAKE HOME POINTS
- Restech’s Dx-pH System is a useful tool in diagnosing non-acid, alkaline reflux, and bile reflux.
- Alkaline reflux is often overlooked, as it is difficult to diagnose.
- With appropriate treatment, bile reflux and its symptoms can be effectively resolved.
TREATMENT
After diagnosis, an adapted treatment was implemented for a non-acid reflux regimen. The patient halted their acid suppression medication and began taking Sucralfate (bile chelator) three times a day, one hour after each meal. The symptomatology improved rapidly with the patient reporting progress within a few days of the medication shift. After four weeks the RSS score was down to 13 (4 + 9 + 0) from a starting point of 37, a decrease of 24 points. Further follow-ups are anticipated to show continued improvement.